- 469-833-2644
Medical Billing and Practice Management: How MedAxis Solutions Helps Healthcare Practices Grow

By the MedAxis Solutions Clinical Operations Team | Updated 2026 | 12-min read
Running a successful healthcare practice today is more demanding than ever. Physicians and providers find themselves hard-pressed to juggle multiple responsibilities all at once, from managing patient care to handling administrative tasks. This can take a toll on healthcare staff while affecting their long-term efficiency and reducing profit margins.
In such a scenario, professional support services like medical coding and billing services and practice management have emerged as a viable option to facilitate healthcare practices.
At MedAxis Solutions, we’ve spent years working alongside healthcare providers to understand exactly where revenue disappears and operational efficiency breaks down. This guide distills key insights into Medical Billing and Practice Management to help optimize your healthcare operations.
What is Practice Management in Healthcare?
In its simplest terms, practice management pertains to the oversight of the day-to-day operational, financial, and compliance-related tasks that keep a facility up and running. Effective practice management isn’t just about filling out forms, but a key differentiator between financially viable practices and those that are struggling to sustain their revenue generation abilities.
Core components include:
- Strategic scheduling that minimizes no-shows and maximizes provider utilization
- Accurate medical billing and coding aligned with current ICD-10 and CPT guidelines
- HIPAA and OSHA compliance systems that protect patients and the practice
- Revenue cycle management (RCM) that tracks every dollar from the first appointment to the final payment
- Human resources frameworks that reduce burnout-driven staff turnover
The Numbers Behind the Problem
Before discussing solutions, it helps to understand the scale of what practices are dealing with:
|
30% of physician time lost to admin tasks |
$99K per physician/year on prior auth alone |
25% average claim denial rate, industry-wide |
65% of denied claims never resubmitted |
It’s worth reflecting that nearly two-thirds of denied claims are simply abandoned. A practice that bills $2 million annually, which could amount to $50,000 to $150,000 in lost revenue every single year.
The Critical Role of Medical Billing and Coding Services: Where Revenue Is Won or Lost
Medical billing and coding services are the financial cornerstone of any practice. When they run well, cash flows are predictable. When they don’t, the entire operation suffers, and the problems compound faster than most practices realize.
What Accurate Billing Actually Delivers
Professional medical billing and coding services don’t just reduce errors. They fundamentally change the economics of running a practice:
- Accurate Claim Submissions: Clean claim rates above 95%, meaning faster adjudication and fewer follow-up cycles.
- Accelerated Reimbursements: Reduced days in accounts receivable (AR), with payments arriving in days rather than weeks.
- Denial Prevention: You are less likely to face denials when systemic issues are identified and fixed proactively, thus protecting your bottom line.
- Regulatory Compliance: Annual compliance with ICD-10 and CPT code updates that change every October and January.
|
Expert Insight “One of the most common issues we see when practices come to us is ‘denial fatigue’ — staff have been dealing with rejections so long that resubmitting starts to feel pointless. But with systematic denial management, the majority of denied claims are recoverable. The revenue is there. It just needs to be pursued properly.”— MedAxis Revenue Cycle Team |
The Real Cost of In-House Billing Errors
A single coding error doesn’t just result in one denied claim. It can trigger a payer audit, flag your practice for increased scrutiny, or in cases of repeated upcoding, even unintentionally, create compliance liability.
The downstream consequences of billing inaccuracy are disproportionate to the original mistake.
Optimizing Revenue Cycle Management (RCM)
Revenue Cycle Management (RCM)https://medaxis.solutions/practice-management refers to a strategic process whereby a patient’s entire financial journey is managed, starting from the moment they book an appointment to the time the provider collects all billable payments.
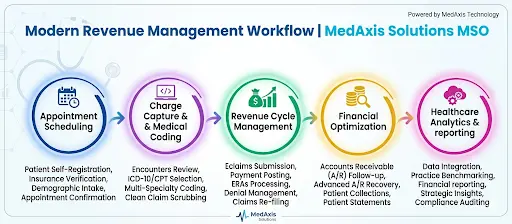
A high-performing RCM system integrates the following tasks:
- Patient Registration & Insurance Verification: Confirm eligibility and benefits before the visit, hence eliminating coverage surprises that delay payment.
- Coding & Billing: Transform provider notes into accurate, compliant claims using the most current coding standards.
- Claims Submission & Payment Posting: Submit clean claims electronically to reduce processing time and minimize rejections.
- Payment Posting & Reconciliation: Record payments accurately and flag discrepancies between contracted rates and actual payments.
- Denial Management: Analyze rejection reasons systematically, appeal recoverable claims, and fix root-cause issues to prevent recurrence
The Operational Challenges Most Practices Don’t Talk About Openly
Understanding the environment healthcare providers operate in today matters — because the challenges are structural, not personal. The hardest-working physicians are still burning out. The most diligent billing staff are still missing claims. Here’s why:
EHR Overload
Physicians average 2 hours of documentation for every 1 hour of patient care. This suggests a cumulative burden that adds up across every working day.
Payer Complexity
Every insurer has different submission requirements, modifier rules, and denial patterns. This knowledge takes years to build and demands constant upkeep to adhere to existing regulatory requirements.
Compliance Volatility
Coding standards, HIPAA requirements, and payer policies are constantly evolving, creating ongoing liability for practices that can’t track every update.
Staff Turnover
Administrative burden is the leading driver of clinical staff burnout, creating a costly cycle of recruiting, onboarding, and retraining.
How MedAxis Solutions Works: Services Built for Real-World Practice Needs
Unlike generalist billing companies, MedAxis is a dedicated Medical Services Organization (MSO) with over 20 years of combined experience in enhancing the operational efficiency of primary care providers.
Our service model is built around your specific workflow, not the other way around.
1. Full-Cycle Medical Billing & Coding
We manage every stage of the billing process: charge capture, coding review, claims submission, payment posting, and denial resolution. Our team is trained on specialty-specific coding nuances and payer requirements, which means fewer errors and faster reimbursements from day one.
2. Revenue Cycle Management
Our RCM service goes beyond billing. We monitor key performance indicators like clean claim rate, days in AR, denial rate, and net collection rate. Furthermore, we provide monthly reporting so you always know where your revenue stands.
3. Insurance Verification & Prior Authorization
We verify patient benefits before appointments and manage the prior authorization process for procedures. This helps reduce delays and prevent the claim denials that often stem from incomplete pre-visit work.
4. Practice Management Support
From scheduling optimization to compliance documentation, our team handles the operational layer so your front desk and clinical staff can focus on patients rather than paperwork.
The Outsourcing Decision: What the Data Says
The most common objection to outsourcing practice management is loss of control. These are critical financial functions. But given below is a breakdown of what in-house management actually costs:
- A full-time billing specialist costs $45,000–$65,000 annually in salary alone, excluding benefits, training, or turnover coverage.
- Denial management requires specialized knowledge that most general billing staff don’t have.
- Compliance monitoring requires dedicated attention that’s difficult to sustain across other responsibilities.
- In-house teams typically achieve clean claim rates of 80–85%; professional billing services routinely exceed 95%.
The economics are strikingly clear: for most practices, outsourcing to a specialized partner recovers more revenue than it costs, with results seen in the first year alone.
Ready to Find Out What Your Practice Is Leaving on the Table?
The first step is understanding your current revenue cycle performance. MedAxis offers a complimentary practice assessment that identifies your highest-impact opportunities, from denial patterns to scheduling inefficiencies, with no obligation.
Schedule Your Free Practice Assessment and get a long-term partner that handles the administrative overload so that you can deliver the highest standards of care.
FAQs
1. What is medical practice management?
Medical practice management involves handling administrative, financial, and operational tasks to ensure a healthcare practice runs efficiently.
2. Why is medical billing and coding important?
It ensures accurate claim submissions, faster reimbursements, and compliance with healthcare regulations.
3. What is revenue cycle management in healthcare?
RCM is the process of managing the financial lifecycle of a patient, from appointment scheduling to final payment collection.
4. How can outsourcing practice management help healthcare providers?
Outsourcing reduces administrative burden, improves efficiency, and allows providers to focus more on patient care.
5. What services does MedAxis Solutions offer?
MedAxis provides medical billing, coding, practice management, back-office support, and revenue cycle management services.
6. How does MedAxis Solutions improve revenue?
By optimizing billing processes, reducing claim denials, and ensuring accurate coding, MedAxis maximizes practice revenue.
